Bridging the gap: exploring the impact of bootcamp on non-technical skills and professional development in early-career orthopaedic trainees | BMC Medical Education

All Orthopaedic trainees (n = 15) commencing ST3 training in the Yorkshire & Humber Deanery in 2019 attended the bootcamp, yielding a 100% participation rate in the study. Pre- and post-bootcamp surveys achieved a 100% response rate. Of the 15 participants, 11 (73%) completed the 2-3-week follow-up interview, and 6 (40%) participated in the 6-month follow-up interview. This substantial reduction in participation at the 6-month point represents a limitation in our ability to draw conclusions about longer-term impacts.
Most trainees rated the Professional Behaviours and NOTSS sessions as relevant to their clinical practice (Fig. 1), indicating their initial receptiveness to non-technical skills training. Post-bootcamp questionnaire responses showed improvements in self-reported competencies across both non-technical and technical domains compared to pre-bootcamp baselines (Fig. 2). Trainees reported increased confidence in recognizing key workplace behaviours, addressing patient safety concerns, and seeking senior guidance for training. Notably, pre-existing awareness of teamwork’s importance in surgical care was already strong among participants, as reflected by minimal change in this specific domain.
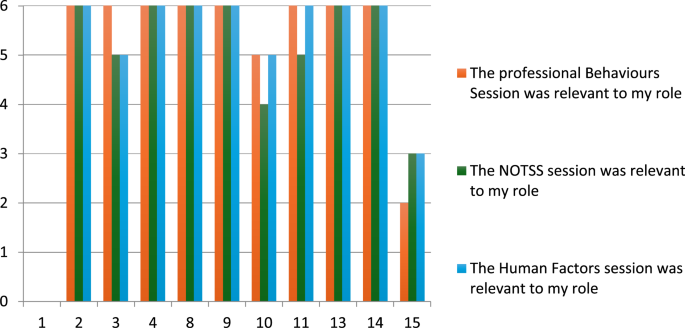
Trainees’ immediate perceptions of non-technical skills during bootcamp
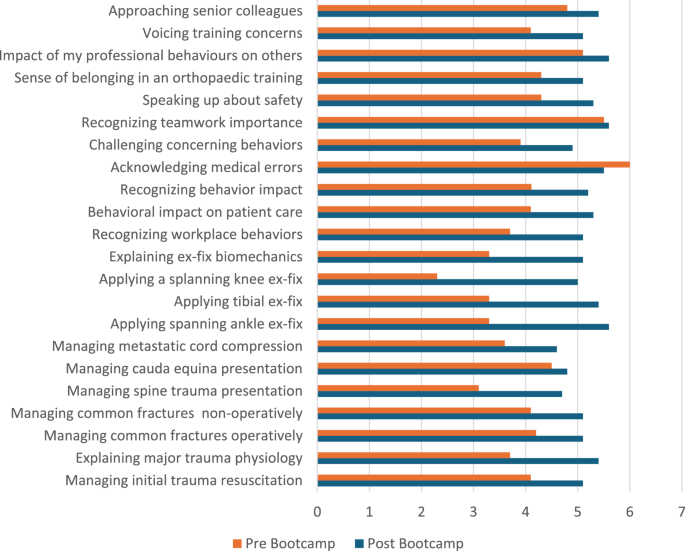
Pre & Post bootcamp scores for behaviours and non-technical skills
Thematic results
Four main themes emerged from our analysis of interviews conducted at 2 weeks and 6 months post-bootcamp: (1) Integration & Expectations, (2) Perception and application of Non-Technical Skills, (3) Psychological Safety & Learning Culture, and (4) Building Relationships.
Theme 1: integration & expectations
The bootcamp served as a crucial orientation mechanism for new surgical trainees, establishing expectations and facilitating integration into the training program. At the 2-week point, participants characterized the bootcamp as a “welcoming introduction” that acknowledged their new status and role in the training program. Participant 1 noted, “It’s somebody’s first experience of training, so it’s important to cover the salient bits and feel at home” (2 weeks), while Participant 13 valued the formal recognition of their new position: “It was nice just to have two days acknowledging you are here, you are on the training programme, here is what we expect of you” (2 weeks).
By the 6-month follow-up, trainees had developed a deeper appreciation for how the bootcamp had initiated their integration into the training environment. Participant 4 reflected, “The bootcamp is great for you as a settling point in terms of what’s available to you, what is expected of you as well as meeting the people and building up a relationship and about settling you into the environment. You have to make the effort in deciding how you want to go on with the training and learn” (6 months).
The bootcamp provided a framework for professional expectations and goals, helping clarify training requirements and pathways. Participant 3 highlighted how it offered “clear goals to work towards and a structured way of going about it” (2 weeks), while Participant 1 emphasized its importance for those transitioning between different training structures: “For me, coming from a non-training to training job, it was important to be told this is exactly what you need for Certificate of Completion of Training (CCT) and this is how to achieve this” (6 months).
A significant finding was trainees’ acute awareness of their outsider status upon entering new training environments. Participant 1 observed, “You arrive in a new region, and some people already know each other—that was certainly the case” (2 weeks), while Participant 13 noted their isolation: “At my hospital, senior registrars had been there before, and many juniors had worked in the deanery previously—I was the only brand-new candidate” (2 weeks).
The informal transfer of knowledge emerged as a key mechanism for transitioning from outsider to insider status. Trainees relied heavily on peer networks and senior colleagues to gain insights into training expectations, departmental culture, and unwritten rules. As Participant 13 described, “It was nice to have someone… a couple of years through the system… a bit of advice about things we should do, things we shouldn’t do, things to look out for…. an acknowledgement you are here, this is what to expect, this is what is going to happen” (6 months).
Theme 2: perception and application of non-technical skills
The data reveals a complex developmental trajectory for NOTSS. Participants progressed from initial skepticism about NOTSS training: “I was initially a bit surprised these topics were in the bootcamp, but it’s probably the best place,” (P1, 2 weeks) to retrospectively acknowledging the value of this training: “The human factors stuff was good; it puts in your head that you are a registrar and going to have to run things…. In hindsight, it was really quite useful, but you don’t realise it at the time.” (P10, 2 weeks). Participant 8 described the bootcamp as an “ignition” for NOTSS awareness rather than a comprehensive training program.
Participants showed a disconnect between their perceived use of NOTSS and their actual application. Multiple trainees described using these skills “subconsciously” without deliberate implementation. Participant 3 stated, “It’s not something in terms of a conscious thing but I’m sure I’ve used them subconsciously,” while Participant 5 noted “I do not always consciously think about the human factors but if I am doing a ward round, I do try and get all the team members involved.”
The data shows progression from passive observation to active implementation. Early after training, participants primarily described watching consultants react in challenging situations, Participant 8 mentions, “I am just focused on what the consultant is doing and how they are reacting.” Many demonstrated incorporating NOTSS into their own practice, particularly in stress management and team communication in theatres, clinics and during on calls – “I am quite conscious to make sure that I am more measured with my responses if I am feeling stressed” (P14, 6months) and “In clinic, if you respect the nurse you work with then you will get along and have a better rapport rather than wanting to get out and it does affect your performance and patient care” (P5, 6 months).
Self-awareness emerged as a particularly valuable component, with participants highlighting the importance of recognizing their own behaviour in stressful situations: “I find myself thinking about when I come to a stressful situation, like when I am operating and there is a section where I don’t know what to do next and get a little bit more stressed, I figure that I become more quiet and I not tend to ask for help” (P4, 6 months).
The transition from SHO to registrar appeared to involve a significant shift in leadership responsibilities, with delegation identified as particularly challenging by a few participants. Participant 14 noted, “As an SHO you don’t really ever delegate you just get delegated to,” and Participant 1 affirmed, “Giving the SHO some freedom and independence is important, but then also being able to tell them when they’ve not done something is too.” Participants expanded their conception of the surgical role beyond technical competence: “I think I’ve been more receptive to the other roles of a registrar. It’s not just about the operative and getting great numbers. There are lots of other aspects of being a registrar that you can use to influence your or others training” (P1, 6 months).
Despite their experiences, participants suggested that the NOTSS component of the bootcamp was too brief: “I wonder if there is feasibility to run an all-day NOTSS course? The sessions gave a brief overview, but it would be good to cover it in more detail” (P9, 2 weeks). Participant 4 observed that non-technical skills “are always there but nobody really describes them, and I think it is good for reflection and things like that” (P4, 6 months).
Theme 3: psychological safety & learning culture
The bootcamp created a supportive learning environment that trainees valued. Participants emphasized how being among peers at similar training stages normalized knowledge gaps. Participant 2 expressed: “You are of similar grade so when they ask you a question you are not looking quite so stupid in front of everyone else” (2 weeks), while Participant 1 acknowledged that “The bootcamp personally for me gave me a bit more confidence” (2 weeks).
This peer-based reassurance was important for trainees who felt isolated in their new environments. Participant 10 highlighted: “The timing of it was good so that you arrive in the following teaching, and you don’t feel like it’s run by ST8s. Especially for someone like me who has come and knows nobody in this deanery. There are other people there that have the same rate of knowledge” (2 weeks).
By the 6-month follow-up, participants reflected on how this early experience had contributed to longer-term confidence. Participant 3 articulated: “It’s where you start in the job, and you feel like am I supposed to be here, am I good enough to be doing this, how I managed to get here—situations where you are a little bit out of depth… I definitely think bootcamp did help me out in terms of as we discussed getting to know everyone and you know what you have got to aim for, and you’ve got a rough timeline of how to get there.”
The data revealed that informal settings significantly enhanced the learning culture. Due to a venue change, one session was relocated to a local pub, creating an unexpectedly productive learning environment. Participant 9 found that “The session (funnily enough in the pub) … was very handy. He talked about portfolio requirements and case based discussions” (2 weeks). Further Participant 10 recounted, “He gave me a tip, for example, fill it out when you are in clinic with your boss, just log in and say, ‘I have filled this out for you do you mind signing it between patients’” (2 weeks).
Similarly, social events fostered relationship-building beyond the clinical or educational context: “The social event on the first evening, it’s always a good excuse to get together… we all started talking to each other outside the work environment” (Participant 7, 2 weeks).
Theme 4: building relationships
Professional relationships were a central component of trainees’ experiences, with the bootcamp serving as a catalyst for network formation. At the 2-week timepoint, participants highlighted the immediate establishment of peer support systems: “The guys whipped out their phones… we made an ST3 WhatsApp group. That group has been buzzing” (Participant 1, 2 weeks). These connections became resources for navigating training challenges, with Participant 13 noting, “If you need some info your first port of call is your colleagues, your other ST3… has anyone done this yet?”.
Beyond horizontal peer relationships, vertical relationships with senior trainees provided crucial insights into career progression and professional development. Participant 4 valued that “Senior trainees give us advice on what to expect and what the road looks like a year or two down the line” (2 weeks), while Participant 13 appreciated seniors’ recognition of their transitional status: “My experience of senior colleagues at bootcamp and at work has been excellent—they acknowledge that you are a new registrar and make room for that” (2 weeks).
By the 6-month follow-up, these initial connections with senior colleagues had evolved into deeper mentoring relationships with significant impact on professional identity formation. Participant 4 reflected on the value of consistent relationships: “I really like working with one particular boss for a whole six months… You get to build a relationship with them, know what they like clinically, what changes their decision-making… but also you get a bit of a show aspect in terms of what life could be as a consultant” (6 months). Participant 14 noted, “Looking at how more senior registrars delegate or how they interact with SHOs… you see different leadership styles and start to reflect on what works well and what does not” (6 months).
Trainees’ perceptions of TPDs shifted from hierarchical authority figures to accessible mentors. Participant 4 expressed: “These guys want to know us; they want to know all about how we are getting on… I think they genuinely do have our best interests at heart” (2 weeks), while Participant 1 noted, “I got the impression they genuinely cared about training and wanted to make sure it is a positive experience” (2 weeks). This transformation lowered communication barriers, with Participant 1 acknowledging, “Previously, I might have been worried about contacting them too often… Now, I feel more confident” (2 weeks).
These relationships influenced trainees’ own leadership development. Participant 1 described: “There was a session on how we see managers and how managers see us, which was really interesting… I definitely have a better understanding of the personality traits and pressures they are under. Personally, I have started to be more accessible and reliable with SHOs” (6 months). Participant 3 observed: “I think you take a lot more on board than you realize. Sometimes, I find myself reacting in a situation in a way that I’ve seen senior colleagues handle it” (6 months).
link